Your head hurts because your Your head hurts because your <anchortext>wisdom teeth are connected</anchor_text> to one of the most powerful nerve networks in your body, and when those teeth push through inflamed, crowded tissue, the pain does not stay politely in one spot. to one of the most powerful nerve networks in your body, and when those teeth push through inflamed, crowded tissue, the pain does not stay politely in one spot. It radiates. That is the short answer. The longer answer involves understanding why eruption triggers this kind of referred pain, how to tell whether what you are feeling is normal or a warning sign, and exactly what you can do about it starting today.
Why Does My Head Hurt When Wisdom Teeth Grow? Causes & Relief

How wisdom tooth eruption actually causes head pain
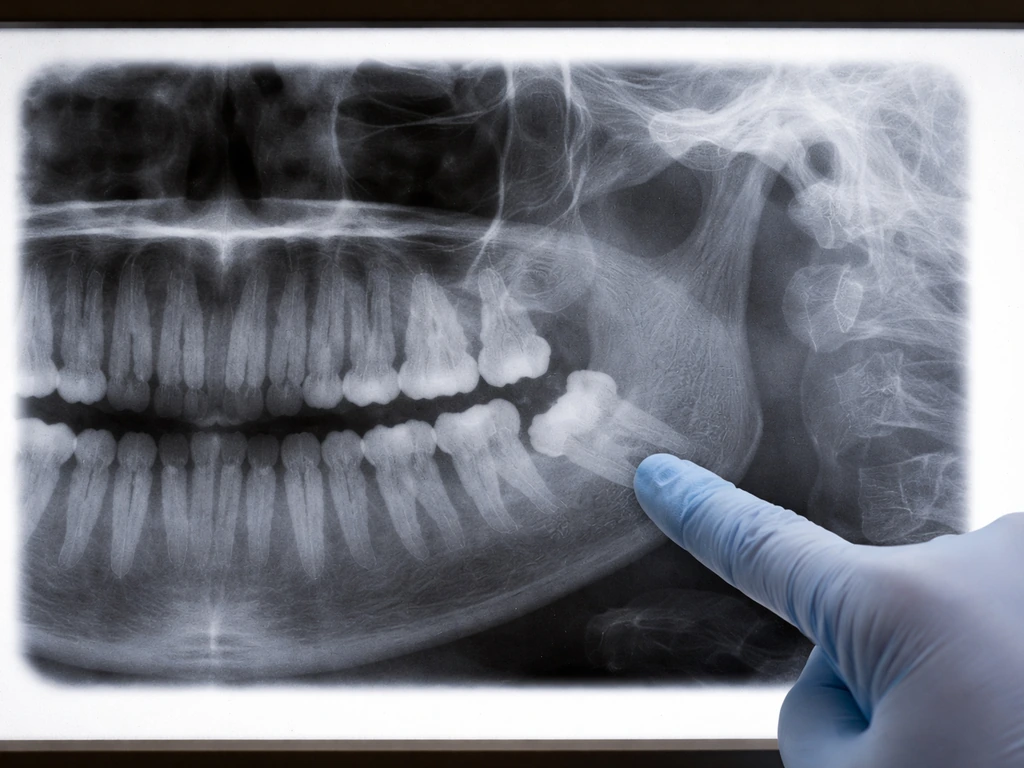
Wisdom teeth (your third molars) erupt at the very back of the jaw, usually between ages 17 and 25, though some people see movement earlier or later. When they start pushing through the gum tissue, they create pressure, inflammation, and microtrauma in a dense area packed with nerves and muscle attachments. That combination is why your head hurts, not just your mouth.
The main culprit is the trigeminal nerve, cranial nerve V. It is the primary sensory nerve for your entire face and oral cavity, carrying pain, temperature, and touch signals from your teeth, gums, jaw, and facial skin straight to your brain. Its mandibular division, called V3, handles sensory input from the lower jaw and lower teeth specifically, which is exactly where most wisdom tooth eruption happens. When tissues around an erupting wisdom tooth become inflamed, V3 fires off pain signals that your brain does not always localize precisely. Instead, you feel aching that spreads to your temple, the side of your head, behind your ear, or even into your neck. This is referred pain, and it is a completely predictable result of how your nervous system is wired.
The trigeminal nerve also controls the muscles of mastication (chewing). When the gum around a partially erupted wisdom tooth is swollen and sore, you instinctively chew differently, hold your jaw tense, or avoid opening your mouth fully. That muscle tension in the masseter, temporalis, and pterygoid muscles compounds the headache and jaw ache. So the pain has at least two drivers: nerve-referred pain from the eruption site and muscle tension from compensating around it.
It is also worth clearing up a myth right here: your gums and the surrounding tissue are not going to regenerate their way around the problem. Some people assume the tissue will simply adapt or 'grow back' to accommodate the tooth naturally, but the biology does not work that way. The gum may cover a partially erupted tooth, creating a flap called a pericoronal flap, but that flap does not resorb or helpfully reshape on its own. It stays, traps food and bacteria underneath it, and becomes a recurring inflammation source unless the situation is actively managed. If you have been reading about dental regeneration elsewhere on this site, this is one of those cases where waiting for the body to fix itself is not a realistic plan.
Normal eruption pain vs. a real red flag
Not all wisdom tooth pain means something has gone wrong. Some discomfort is a completely expected part of eruption. The problem is that the line between 'normal and annoying' and 'you need to call a dentist today' can feel blurry when you are in the middle of it. Here is how to tell them apart.
What normal eruption pain looks like
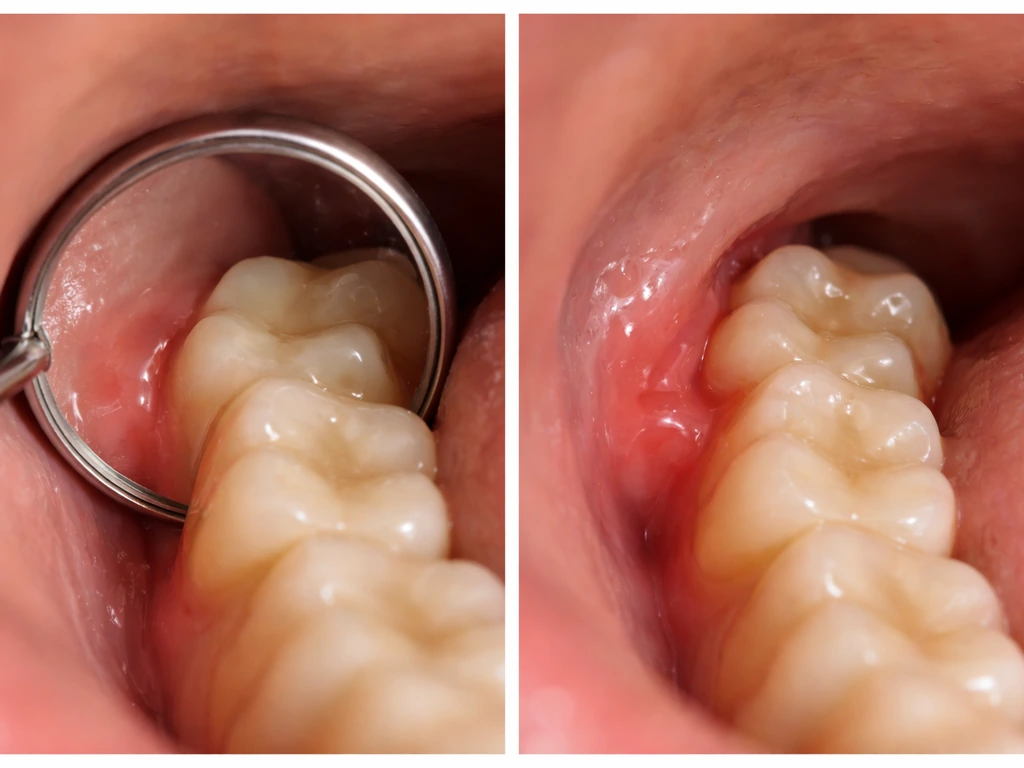
- Mild to moderate dull aching or pressure at the back of the jaw
- Tenderness in the gum directly over or behind the emerging tooth
- Slight swelling of the gum tissue in that specific area
- A low-grade headache on the same side, especially after eating or clenching
- Pain that comes and goes over days or weeks as the tooth slowly moves
- Mild sensitivity that improves with over-the-counter pain relievers
Red flags that signal a complication
The following symptoms are not part of normal eruption. Each one warrants a dentist call, and some warrant urgent care if your dentist is not immediately available.
- Pericoronitis: infection under the gum flap covering a partially erupted tooth. Signs include throbbing pain, visibly swollen and red gum tissue, pus or a bad taste, fever, and difficulty opening your mouth (trismus). The trigeminal nerve pathways mean this can cause severe head and neck pain that feels out of proportion to what you can see in the mirror.
- Impaction: when the wisdom tooth is angled or blocked and cannot fully erupt. Pain can be intense, persistent, and may involve the ear or jaw joint. An impacted tooth often only shows up clearly on an X-ray.
- Dry socket (post-extraction): if you have had a wisdom tooth recently pulled and the pain is getting worse rather than better after 3 to 4 days, especially with a bad smell or taste, this is dry socket. It is not a normal part of healing.
- Spreading infection: fever above 101°F (38.3°C), visible swelling under your jaw or in your neck, difficulty swallowing, or swelling that is closing off your throat are emergency signs. Go to an emergency room, not just urgent dental care.
- Numbness or persistent tingling in your lip, chin, or tongue may indicate nerve involvement from an impacted tooth pressing on the inferior alveolar nerve.
Common symptoms and when they tend to start

Wisdom tooth eruption does not happen overnight. The tooth moves in stages over months or even years, and pain flares tend to follow that pattern. Many people have their first notable discomfort when the tooth is just starting to poke through the gum surface, a phase where the gum is partially open but the tooth is not fully through. That partial opening is the most trouble-prone period because it creates a small pocket that traps food and bacteria.
| Symptom | Typical onset | What it usually means |
|---|---|---|
| Dull jaw pressure | Early eruption, often intermittent | Normal tissue displacement as the tooth moves |
| Gum soreness at the back of the mouth | When tooth begins breaking through the surface | Normal eruption inflammation |
| Headache on one side | During active eruption phases | Referred pain via trigeminal nerve, often worsened by muscle tension |
| Ear ache or jaw joint ache | With partial eruption or impaction | Referred pain from V3 or TMJ involvement from altered chewing |
| Swollen, red gum flap with bad taste | After partial eruption with food trapping | Pericoronitis, needs dentist evaluation |
| Fever and difficulty opening mouth | With progressing infection | Advanced pericoronitis or spreading infection, urgent care needed |
| Worsening pain 3–5 days after extraction | Post-extraction | Dry socket, call your dentist same day |
What you can do at home in the next 24 to 72 hours
If your symptoms look like normal eruption pain and there are no red flags, these steps will genuinely help. They are not just 'be patient' advice. Each one targets a specific part of the pain cycle.
Pain relief
Ibuprofen (Advil, Motrin) is generally the better choice over acetaminophen for pain when new teeth grow because it handles both pain and inflammation, which is the root driver. pain when new teeth grow Take it with food, follow package dosing guidelines, and do not wait until the pain is severe. It works better when taken on a schedule for the first 48 hours rather than on demand. If you cannot take NSAIDs (due to stomach issues, kidney problems, or blood thinners), acetaminophen is your alternative. Do not combine both without talking to a pharmacist or doctor first unless you have been specifically advised to do so.
Saltwater rinses

Warm saltwater rinses are one of the most effective and accessible things you can do. Dissolve half a teaspoon of table salt in 8 ounces of warm water and gently swish for 30 to 60 seconds, focusing on the back of the affected side. Do this after every meal and before bed. The saline solution helps clear debris from the eruption site, reduces bacterial load, and soothes inflamed tissue. Do not rinse aggressively, a gentle swish is enough. If you have had a tooth extracted recently, avoid forceful rinsing for the first 24 hours to protect the clot.
Cold and warm compresses
In the first 24 to 48 hours of a flare, a cold pack applied to the outside of your jaw for 15 to 20 minutes at a time helps reduce acute swelling. After the initial inflammation phase (roughly 48 hours in), a warm compress can help relax the jaw muscles contributing to your headache. Do not apply heat to an active infection as it can draw more blood flow to the area and worsen swelling.
Gentle cleaning
It might feel counterintuitive to brush near a sore area, but keeping the eruption site as clean as possible is critical. Use a soft-bristled toothbrush and gently clean around and behind the erupting tooth. A water flosser set to low pressure can help flush the area under any gum flap without traumatizing tissue. If you have an oral irrigator, use it after meals. Do not poke at the area with your finger or any object, and avoid the temptation to try to lift or pull back the gum flap yourself.
What not to do
- Do not smoke or use tobacco products. Smoking significantly increases infection risk and delays healing.
- Do not drink through a straw if you have had a recent extraction (dry socket risk from suction pressure).
- Do not apply aspirin directly to the gum tissue. This is an old home remedy that causes chemical burns, not relief.
- Do not ignore worsening symptoms hoping they will resolve. Normal eruption pain fluctuates but should not steadily escalate.
- Do not take antibiotics from a previous prescription on your own. They may not be the right type, and self-prescribing contributes to antibiotic resistance.
When to call a dentist or go to urgent care
Call your dentist within 24 to 48 hours if your pain is not improving with the home steps above, if you see visible pus or swelling extending beyond the gum, or if you are having trouble opening your mouth fully. Trismus (limited mouth opening) is one of the clinical signs of pericoronitis spreading into the muscles, and it reflects trigeminal nerve involvement plus masticatory muscle inflammation. It is not something to wait out.
Go to urgent dental care or an emergency room same day if you have a fever, swelling under your jaw or neck, difficulty swallowing or breathing, or pain so severe it is not touched by normal doses of OTC pain relievers. A spreading dental infection can become serious quickly, and this is one area where 'it will probably clear up' is not the right bet.
When you arrive at the dentist, expect a visual exam of the eruption site, probing around the gum flap to check for pocket depth and tenderness, and almost certainly an X-ray (panoramic or periapical) to see how the tooth is positioned, whether it is impacted, and whether any adjacent teeth or bone are affected. This is the only reliable way to know what is actually happening under the surface.
Treatment options your dentist may recommend
Treatment depends entirely on what the exam and X-ray reveal. There is no one-size-fits-all answer, but here are the most common paths.
Deep cleaning around the erupting tooth
If pericoronitis is the issue but the infection has not spread, a thorough professional cleaning to irrigate and debride the area under the gum flap is often the first step. Your dentist may use a dental pick, syringe irrigation, or an ultrasonic scaler to flush out food debris and bacterial buildup. This alone often brings significant relief within 24 to 48 hours.
Prescription rinses and antibiotics
Chlorhexidine gluconate rinse (a prescription-strength antimicrobial) is commonly prescribed after a cleaning to keep the area suppressed while it heals. Antibiotics are prescribed only when there are signs of spreading infection, fever, or systemic involvement. They are not a routine part of wisdom tooth eruption management and should not be expected as a given. When they are needed, amoxicillin is the most common first choice, with alternatives for penicillin-allergic patients.
Extraction considerations
If the wisdom tooth is impacted, has caused repeated pericoronitis episodes, is damaging adjacent teeth, or has no realistic path to full eruption, extraction is typically the recommended long-term solution. This is especially true for lower wisdom teeth that are partially erupted with a persistent gum flap. No amount of cleaning prevents the flap from being there, and repeated infections in the same spot are a signal that the tooth needs to come out. Some dentists will stabilize an acute infection first before extracting, because operating in an infected field has its own risks.
One more myth worth addressing: extracted wisdom teeth do not grow back. There is no biological mechanism for third molar regeneration in adults, and this is a firm biological limit. If you have been wondering about this after reading about dental regeneration, the short answer is that adult permanent teeth, once extracted, are gone. The body does not replace them.
How long this lasts and how to reduce future flare-ups
Normal wisdom tooth eruption discomfort, without complications, typically lasts a few days to a couple of weeks per episode, with quiet periods in between as the tooth moves in stages. Full eruption of a wisdom tooth that has a clear path can take months to over a year from first symptoms to the tooth fully in position, so if you’re asking how long does wisdom tooth take to grow, that timeline can help you set expectations. Pericoronitis episodes, if that is what is happening, often recur until the situation is definitively managed.
For reducing future flare-ups while a wisdom tooth is still in the process of erupting, the most effective strategies are consistent oral hygiene around the eruption site (including after every meal), regular dental check-ups so the tooth's progress can be monitored, and not delaying a dentist visit when symptoms escalate. Staying on top of monitoring means you catch impaction or repeated infection early, before they create bigger problems.
If you have already had one wisdom tooth removed and are wondering about the remaining ones, each tooth should be evaluated individually on its own position, eruption path, and symptom history. There is no rule that all four must come out, but there is also no natural regeneration or self-correction process that will fix an impacted or chronically inflamed site. The biology is what it is, and having a dentist track it with periodic X-rays is the most practical way to stay ahead of problems rather than reacting to them.
FAQ
Can a wisdom tooth headache feel like a migraine, and how do I tell the difference?
It can feel similar because referred pain from the trigeminal nerve can hit the temple or behind the ear. A practical clue is timing and triggers, eruption flares often track chewing, gum tenderness, or a partially opened gum flap, and they worsen when food gets trapped near the back molar. True migraine often comes with nausea, light sensitivity, or a consistent pattern not tied to mouth opening or local gum soreness.
Why does it hurt more when I chew on that side, even if my tooth does not look infected?
Chewing increases pressure and muscle load around the erupting area, so inflamed gum tissue under a partially covering flap and jaw muscles tense more. Even without visible pus, that pressure can irritate the nerve endings connected to the jaw, which is why the pain can be sharp or throbbing during mastication.
Is it normal to get bad breath or a bad taste with erupting wisdom teeth?
Yes, it can happen when food debris and bacteria get trapped around a partially erupted tooth, especially during pericoronal flap stages. The key difference is trajectory, if the smell or taste improves after rinses and cleaning but returns quickly, it suggests ongoing pocketing that still should be monitored by a dentist.
What if the pain is mostly in my upper teeth or behind my ear, can a lower wisdom tooth still cause that?
Yes. Referred pain can travel to nearby structures because the trigeminal nerve branches overlap sensory input patterns. Upper or ear-area discomfort does not rule out a lower wisdom tooth issue, but if you also have ear fullness, drainage, or hearing changes, get evaluated promptly because those can point to non-dental causes.
Should I avoid brushing or flossing around the erupting wisdom tooth to prevent more pain?
No, gentle cleaning usually helps more than it hurts. Use a soft-bristled brush and careful technique, then rinse afterward. Avoid aggressive digging, and if a water flosser hurts, lower the pressure or stop and ask a dentist how to clean that specific spot.
How soon should I take ibuprofen after the flare starts, and can I take it more than once per day?
Start at the first sign of a flare rather than waiting until pain becomes severe, it tends to work better when inflammation is still ramping up. Follow the package dosing limits and do not exceed the daily maximum. If you have kidney disease, a history of stomach ulcers, or you take blood thinners, ask a clinician before using NSAIDs.
What symptoms mean I might have pericoronitis or a spreading infection instead of just normal eruption pain?
Look for worsening rather than gradually easing pain, visible swelling around the gum flap, pus, fever, trouble opening your mouth, and difficulty swallowing or breathing. Another red flag is pain that is not controlled by normal OTC doses, especially if it keeps escalating over hours.
Can I use a warm compress or heat after 48 hours if the area still feels tender?
Yes, warm compresses can help relax masticatory muscles after the initial inflammation phase. Avoid heat if you suspect an active infection with spreading swelling, instead stick with gentle rinses and cold packs until you can be assessed.
Is it ever okay to try to lift the gum flap myself or rinse more forcefully to clear it out?
No. Lifting the flap or poking the tissue increases trauma and can worsen inflammation or introduce bacteria deeper into the area. Use gentle swishing only, and if food is trapped, rely on dentist cleaning or a low-pressure irrigator technique.
How long should I wait before scheduling a dentist visit if the pain is there but not severe?
If it is not improving within 24 to 48 hours of home measures, or if it keeps returning in the same spot, schedule a visit rather than watching it for weeks. Recurrent pericoronitis or a persistently tender flap is a sign that monitoring alone may not be enough.
If one wisdom tooth was removed, why might the remaining ones still cause headaches?
Because each third molar can have its own eruption path, flap pattern, and risk of impaction or pocketing. A tooth that partially erupts can recreate the same nerve referral and muscle tension cycle even if the other side is gone, which is why the remaining teeth should be evaluated individually with X-rays.
Do imaging and exams matter if my symptoms already match “normal eruption”?
Yes, because X-rays and probing can confirm whether a tooth is impacted, how close it is to adjacent roots, and whether there is a deep pocket or active pericoronitis. Symptoms can overlap with other issues, like cavities on neighboring molars or unrelated jaw problems, so an exam prevents missed causes.
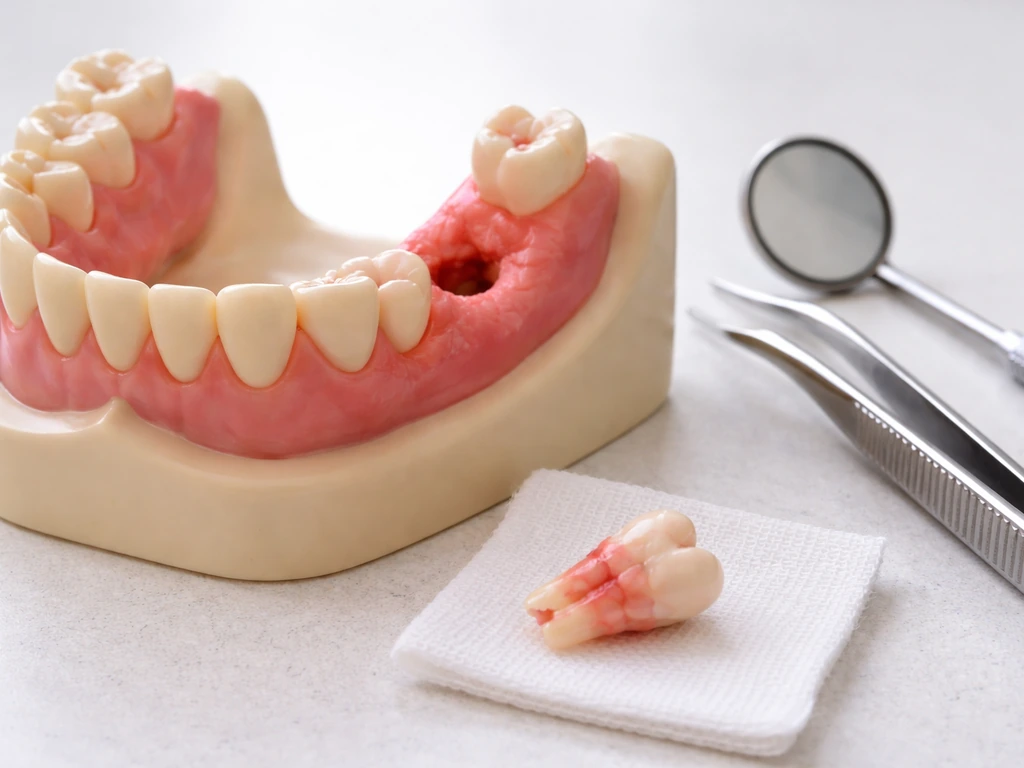
Answer if wisdom teeth can grow back after extraction, why it seems so, rare exceptions, and next steps.
Learn how long wisdom teeth take to erupt, what delays growth, and when to see a dentist for impaction or pain.
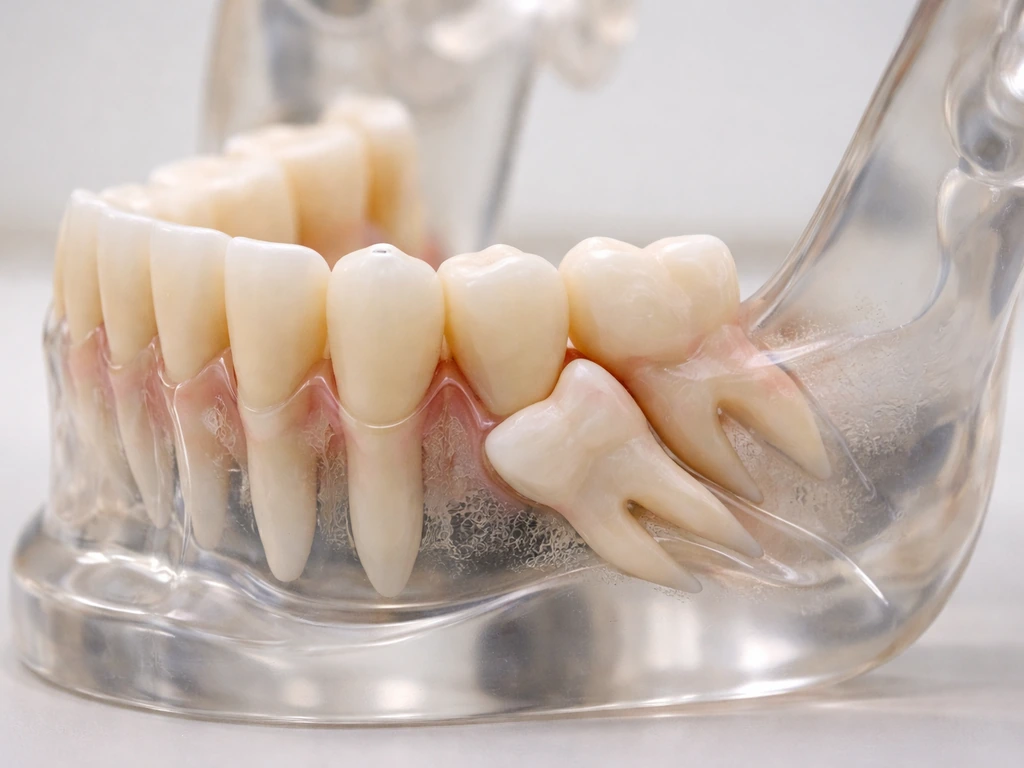
Learn why wisdom teeth grow sideways, what complications to expect, and next steps like X-rays, monitoring, or extractio

